
Leishmaniasis and Leishmania
Leishmaniasis is infection with a trypanosome parasite of the Leishmania genus. Trypanosomes are a protozoan parasite. Protozoan parasites are microscopic one celled parasites. Trypanosomes are all parasites and are primarily found in insects, but several have life cycles that involve additional hosts. A host is an organism infected by a parasite. Primary/definitive hosts are the natural host where the parasite reaches adulthood and reproduces, secondary/intermediate hosts may be required for a developmental stage of the parasite, and aberrant hosts are hosts which are accidental and are not a normal part of the parasite’s life cycle. Other trypanosomes cause sleeping sickness and Chagas disease. Leishmaniasis (the disease condition) is caused by over 20 species of Leishmania (the parasite).
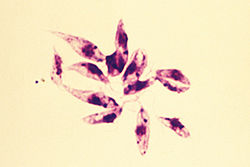
Leishmania tropica
Leismania infection is contracted through the bite of an infected sandfly. There are at least 93 species of sandfly worldwide known or suspected to be vectors of the leishmaina parasite. This parasite has a long history, ancient accounts document leismaniasis (but not by that name) as early as the 7th century BC. Ancient relatives of leishmania have been found in fossilized sandflies. The causative agent of leishmania was only identified in 1901 when parasites were discovered inside the cells of infected human organs.
Leishmania is transmitted by the bite of an infected sandfly and in the cutaneous form produces open sores at the bite location that heal in several months to a year. Diffuse disease may resemble leprosy. The visceral form is the most serious form, causing fever and damage to the spleen and liver, and is potentially fatal if untreated. At the site of the bite the parasites are consumed in their promastigote form by macrophages (one of the immune cells whose job is to ‘eat’ pathogens). Once inside the macrophage the parasite larvae transform into amastigotes and multiply. These transformed larvae may travel through the host or be consumed by a sand fly when it ingests infected macrophages. Once in the sand fly the parasite transforms again into the promastigote form and multiplies before traveling through the sand fly to the mouthparts to begin the cycle anew. Leishmania is identified by looking at the parasites on a blood sample from an infected person.

Leishmania inside of a macrophage. The pink stuff is the parasite and the blue is the cell.
Leismania affects around 12 million people in 98 countries, with 88 countries having endemic leishmania populations. Leishmania is present in the Americas, Africa, and Asia. Many new cases are identified each year. Depending on location leishmania can be something only contracted by unlucky tourists, or something endemic to (naturally occurring in) the area and causing localized epidemics (a widespread occurrence/outbreak of a disease). In 2012 an epidemic of cutaneous leishmaniasis occurred among Syrian refugees in Lebanon. Most people affected in this epidemic were younger than 18 years old, affected persons had arrived from endemic and non-endemic areas. Predisposing factors that contributed to this outbreak were poor housing conditions that provided inadequate sanitation, waste disposal, and insulation. Poverty, malnutrition, population displacement, weakened immunity, and poor housing are risk factors for leishmaniasis. These risk factors make leishmaniasis a humanitarian/human welfare concern as well as a communicable disease issue.
As environmental changes occur putting humans in closer contact with sandflies the risk for leishmaniasis increases. Deforestation, building dams, and urbanization are associated with increases in leishmaniasis occurrence. In many instances people infected with the parasite may undergo a long period without signs of disease. Humans are a main reservoir of the disease, meaning the sand flies get the parasite from humans and transmit it to other humans, in many locations; however, in some areas other reservoirs exist such as dogs and rodents. The interactions between humans and other reservoir species and between humans and the environment contribute to exposures and overall incidence levels of the disease.

Sandfly
Earlier cutanous leishmaniaisis was mentioned, this is when leishmania affects the skin. There is also visceral leishmaniasis, when leishmania affect the internal organs (viscera), and mucocutanous leishmaniasis, when the mucous membranes of the mouth, nose, and throat are affected. Visceral leishmaniasis is an example of one health as it is both anthroponotic (humans to animals) and zoonotic (animals to humans). In Brazil previous programs focused on control of the disease by culling of infected dogs; currently efforts are being made to preventatively vaccinate dogs, this results in better compliance from humans with the preventative measures and has reduced the incidence of disease in both dogs and humans. Despite the vaccine for dogs (which only covers one species of leishmania and has confounding factors beyond the scope of this lesson), human vaccines are still in production and not available.

A dog with signs of visceral leishmaniasis
Prevention and control of this disease depends on early diagnosis and disease surveilance, controlling the vector and reducing exposure to it. Controlling the animal vectors when applicable, and obtaining cooperation of other local organizations in the above effort. The World Health Organization is involved in Leishmaniasis control efforts.











 Leishmania tropica
Leishmania tropica Leishmania inside of a macrophage. The pink stuff is the parasite and the blue is the cell.
Leishmania inside of a macrophage. The pink stuff is the parasite and the blue is the cell. Sandfly
Sandfly A dog with signs of visceral leishmaniasis
A dog with signs of visceral leishmaniasis
















